I wore my son’s insulin pump for a week—and here’s what I learned about living with type 1 diabetes
Six years ago I didn’t know insulin pumps existed. I’d never seen one, never contemplated how the 1.25 million Americans with type 1 diabetes managed their health, didn’t think about diabetes at all.
And then, at 20 months of age, my son, Tom, was diagnosed with type 1 diabetes. It was like being struck by lightning — there was no family history of the disease, an autoimmune disorder that kills pancreatic cells and destroys the body’s ability to absorb life-sustaining glucose. The round-the-clock regimen of blood sugar tests and insulin injections shocked us into an alternate reality.
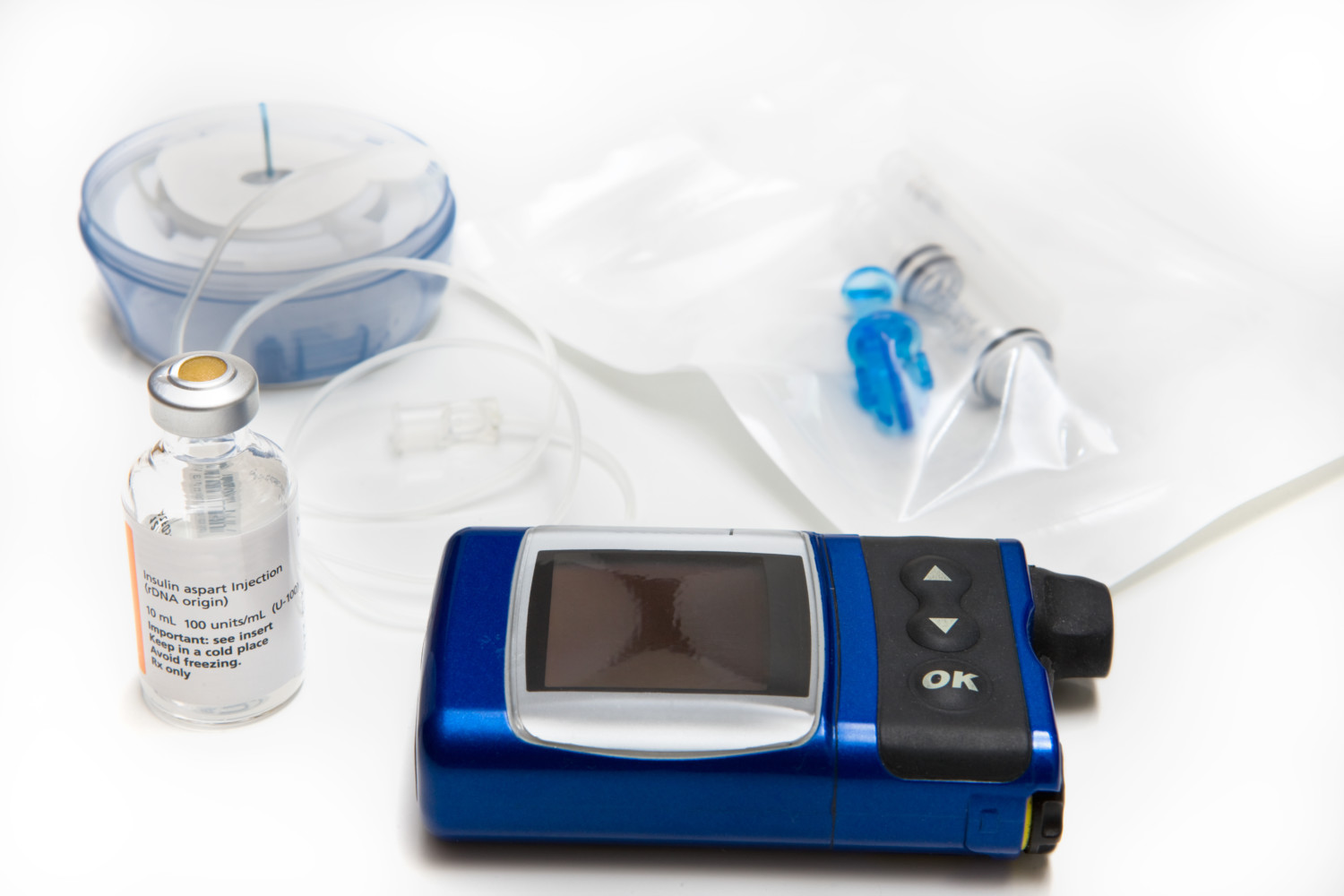
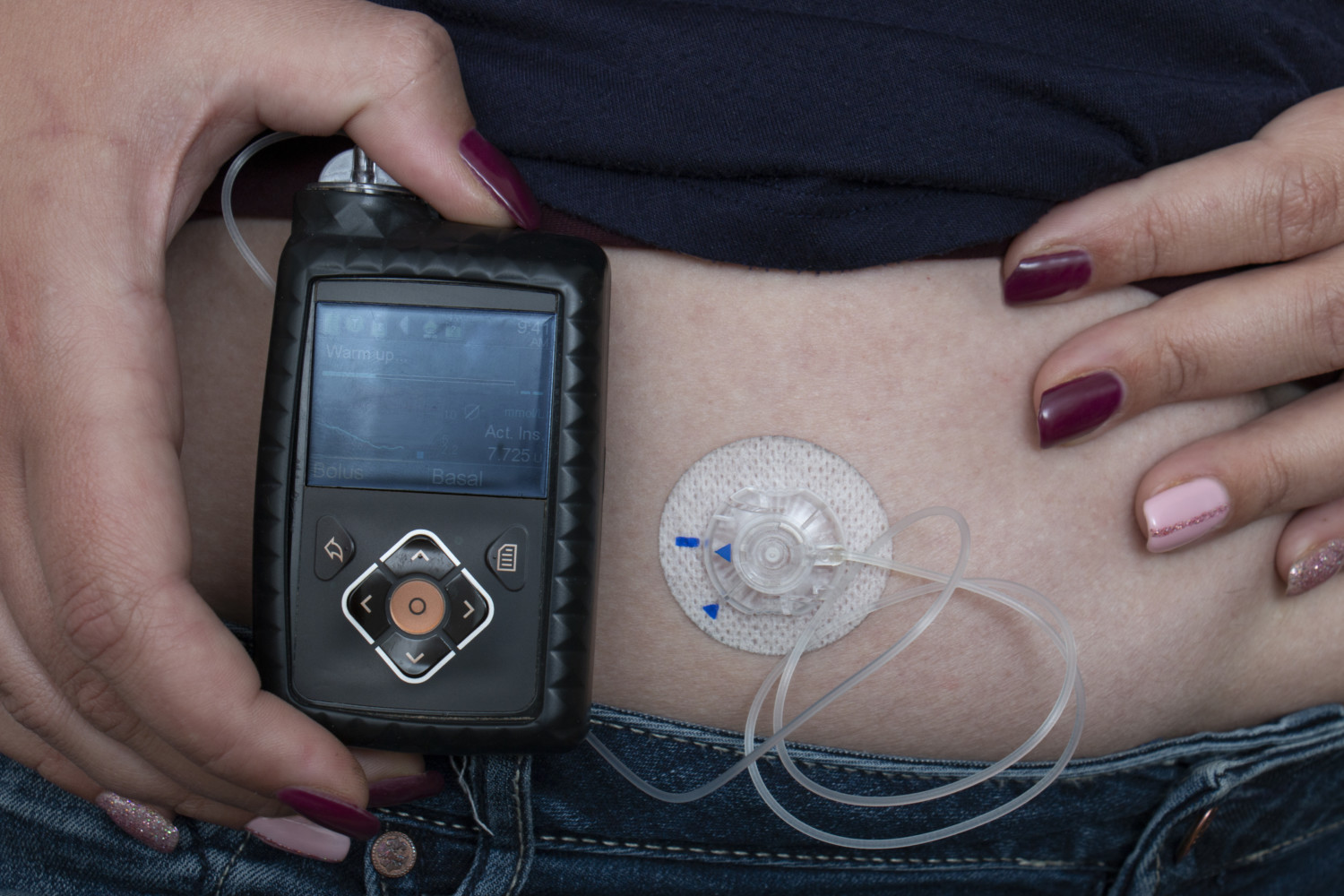
Then, two years after diagnosis, we started him on the pump, which is what he still uses today at age 7. It’s essentially a small, wearable IV machine like you’d see in a hospital. The pump is filled with insulin, which it dispenses into his body through tubing and a cannula (a smaller tube) under his skin. This way, patients don’t have to inject themselves with syringes multiple times daily and can just give insulin through the tube.
MORE: NFL player Mark Andrews helps save woman’s life mid-flight with diabetic test kit
Tom wears his pump all day, every day, only removing it to bathe or swim. When the warranty on his first pump expired, we switched to another brand and I got the idea: What if I wore Tom’s old pump for a while, just to see what it’s like?
I saved a few supplies from the old pump, snagged some sterile saline, and once we booted up the new system I gave it a try. Here’s what I learned from my week on an insulin pump:
It hurts
Tom has always preferred we use a topical anesthetic when changing the pump’s infusion set — the cannula and connection to the pump that must be switched out a few times a week.
I understood why he’d want the anesthetic. The needle used to insert the cannula is pretty intimidating-looking, though very thin and flexible. But I’d often find myself gritting my teeth while applying the numbing cream. “We’ve done this hundreds of times now. Can we just do the change and get it over with?” I’d think with a sigh.
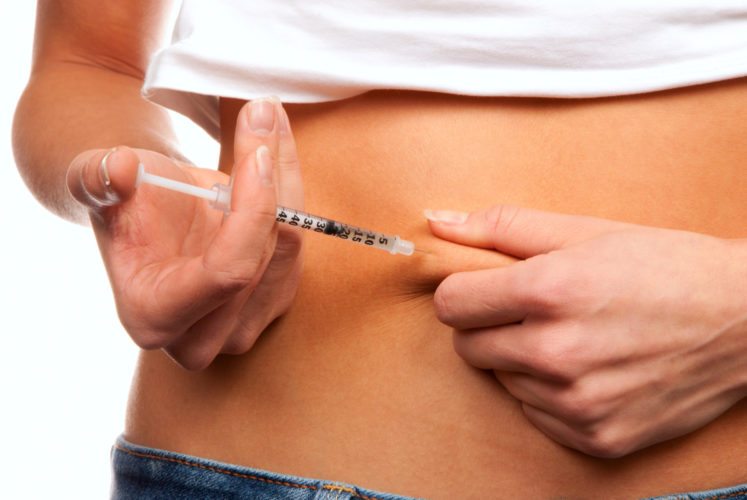
When I put in a set for my pump experiment, I got my comeuppance. I invited Tom to watch while I injected a fresh cannula under the skin on my belly, sans anesthetic.
Oof. I yelped as soon as the needle clicked into place, only to yelp again as I removed it. The cannula stayed under my skin where it belonged, and felt like a tiny stab every time I moved. Tom looked smug.
The pain retreated over the next couple days, but the set still gave me a little zing of a sting anytime it got bumped. I changed the set one more time during my week pumping saline and it hurt way less when inserted; I wondered if I went too deep with the first one.
Still, the second set also zapped me with pain when it got too big of a bump. I finally understood Tom’s frequent complaints that “my pump hurts,” even when his skin didn’t look irritated and all seemed well.
The Tubing Can Be A Hassle
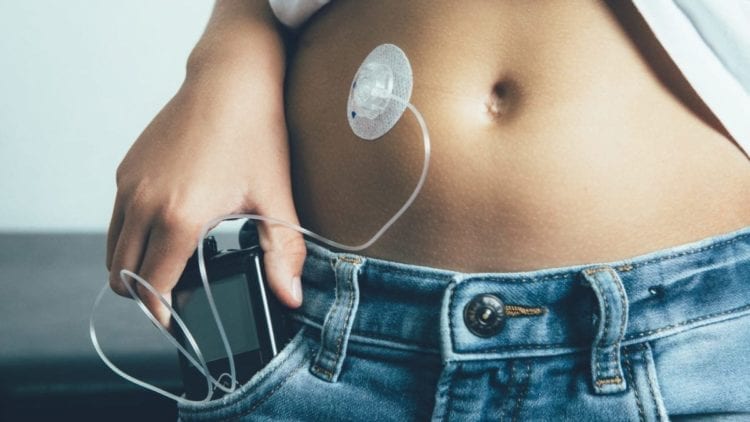
I kept the pump in my pants pocket with the tubing running up under my shirt. I’d seen a few adult insulin pumpers wear theirs this way, but Tom liked to keep his in a little fanny pack at his waist.
I could quickly see why. I snagged my tubing on various doorknobs and nearly ripped out the set a couple of times. At night, the pump fell out of my carefully selected shorts-with-pockets and got wrapped around me. Going to the bathroom was a dance with the devil: If I forgot to remove the pump and hold it in my hands before going, there was a chance it could plop out of my pocket and into the toilet.
As a kid who fancies himself a future Spider-Man, Tom had the right idea all along.
Being Hooked Up To A Machine All The Time Stinks
I did my best to use the pump as if I actually needed it: I wore it at all times, except for showering. I changed the infusion set on schedule. I gave myself a bolus (i.e., a dose) of my faux-insulin after each meal.
I caught a glimpse of the discomfort and worry of being constantly attached to a medical device. I got why some people with type 1 prefer to remain on injections — for all the convenience of it, the pump is ever-present by necessity. You’re always tethered.
Still, because I don’t have type 1 for real, the experience was incomplete. I could take the pump off, stow it in a closet and never think about the damn thing again. My son does not have that luxury. He never will, at least not in the foreseeable future. That’s the part that breaks my heart. This is forever.

Right now I do all of his carbohydrate-calculating, bolus-giving and pump-changing. I’m the one who wakes up in the middle of the night when his low-blood-sugar alarm bleats. I know diabetes. But I tried as best I could to walk in his shoes for a week, and I still don’t really know his life with diabetes.
I’ve never felt the dread and fear that comes with dangerously low blood sugar. I’ve never had my blood glucose levels shoot dangerously high, or experienced the horrible, unquenchable thirst that comes with it. I’ve never had to confront the knowledge that without constant access to the right medication, I will die.
What I do know is that my son is happy in spite of the challenges of type 1 diabetes. He’s hilarious. He loves to run and roughhouse just like any other 7-year-old kid. He’s smarter than he knows. One day he’ll take over diabetes care for himself and I’ll be on the sidelines rooting for him.
No one’s sure when or if a cure for type 1 will be found. But I hope I get to see the day when Tom can take off his insulin pump, stow it in the closet and never think about the damn thing again.