These Medications Should Never Be Mixed With Alcohol
Drinking alcohol while taking medication may seem like no big deal, but combining the two can often be very dangerous.
If you’ve been prescribed medication and aren’t sure if it’s safe to drink that red wine, you might want to think twice about hitting the bottle. There are more than 100 medications that can cause issues when mixed with alcohol.
Combining them can include symptoms that range from something as minor as nausea to more serious complications, like organ damage, stomach bleeding, difficulty breathing and even death.
One study from the National Institutes of Health (NIH) found that 42% of people who drink alcohol were taking medication that could negatively react with the drink. So how do you know what is dangerous to mix with booze and what’s not?
Here’s a list of medications that should never be mixed with alcohol, along with some of the possible health risks. It should be noted that the risks vary based on the exact type of medication.
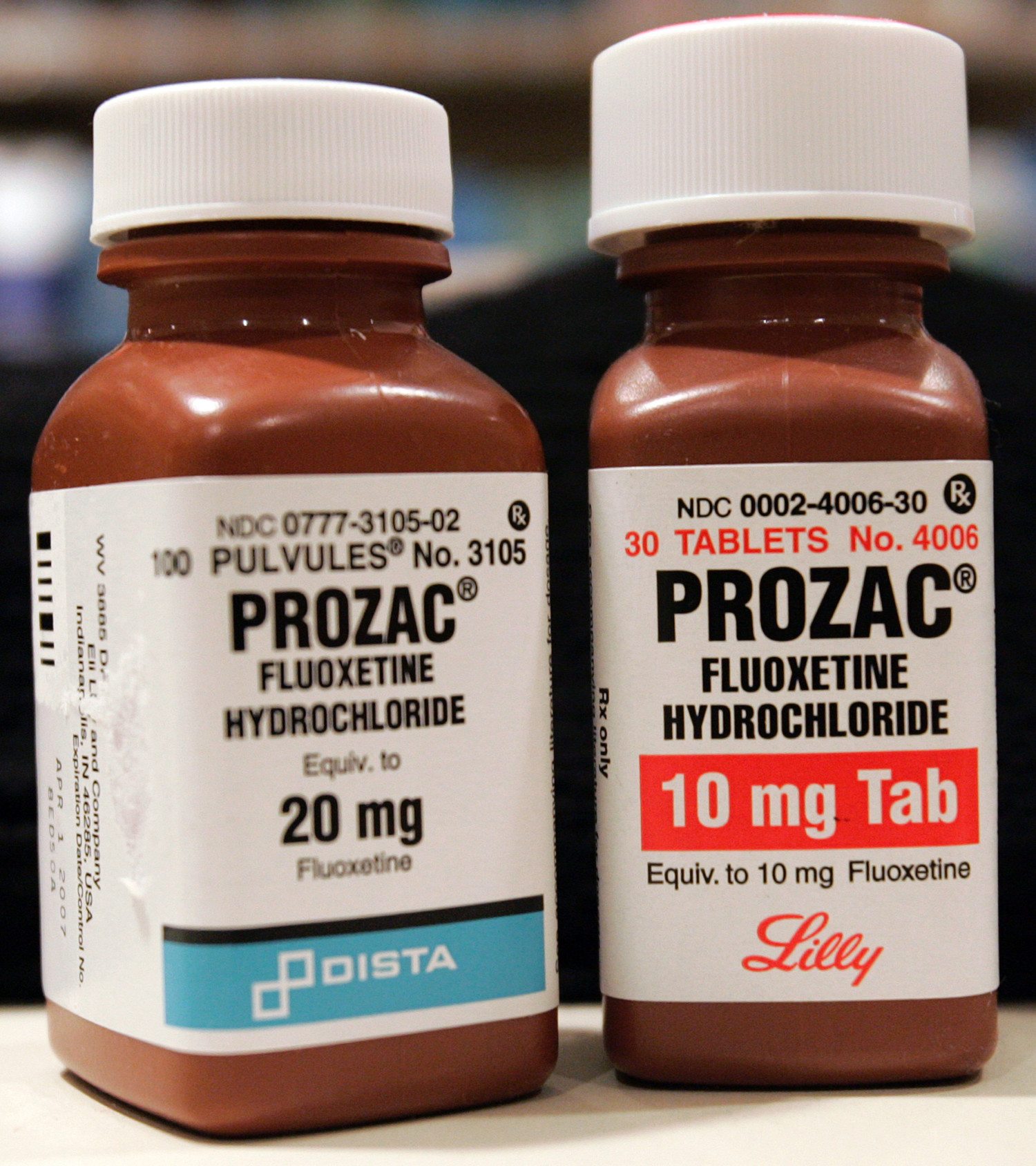
1. Anti-anxiety drugs (such as Xanax, Valium and Ativan) and anti-depression meds (such as Prozac, Wellbutrin and Zoloft)
Risks include: Drowsiness, dizziness, risk of overdose, risk of high blood pressure/heart attack, breathing difficulty, impaired motor control, liver damage, memory problems and unusual behavior
2. Antihistamines and other allergy medications (such as Zyrtec and Benadryl)
Risks include: Drowsiness, dizziness and increased overdose risk
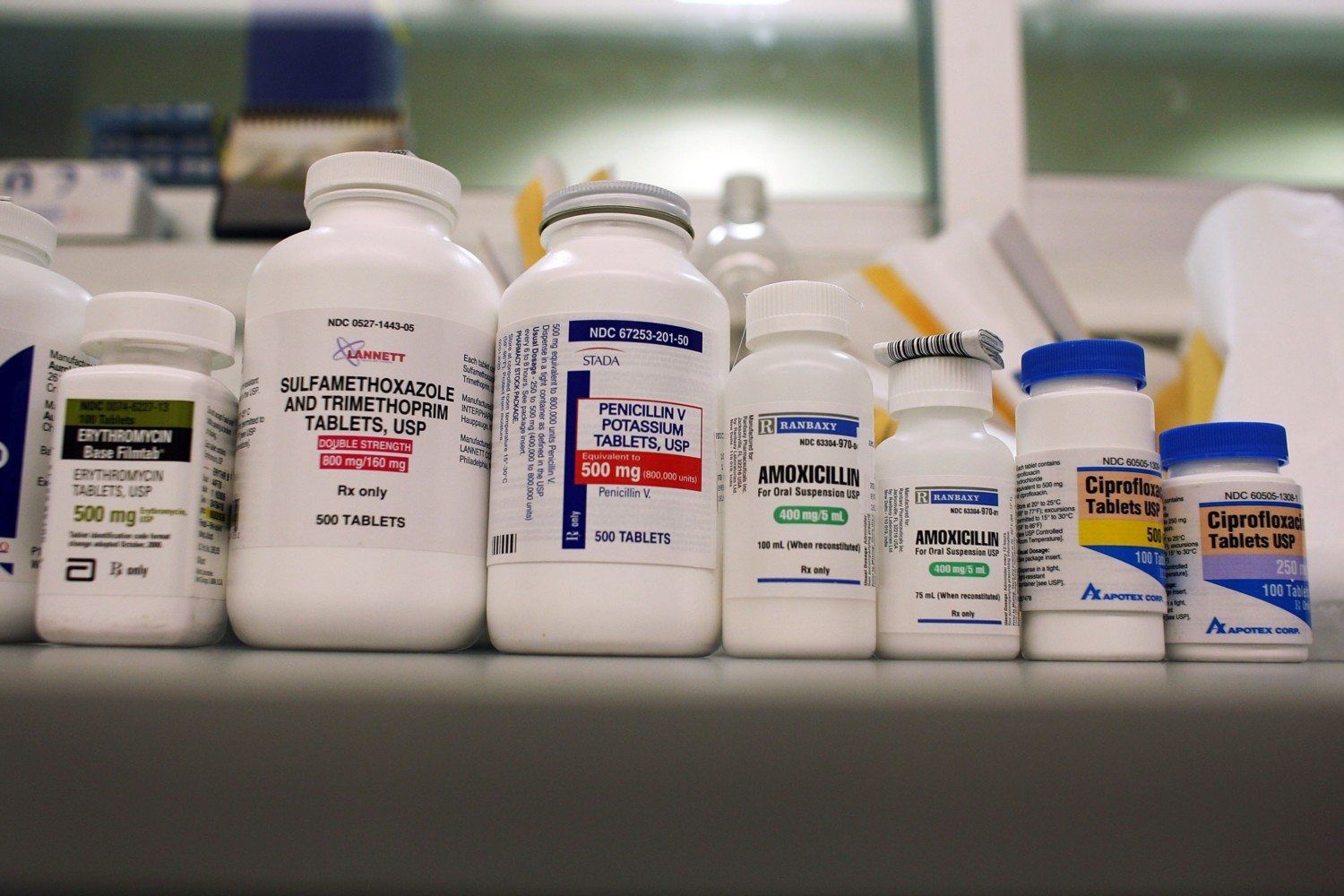
3. Antibiotics
Risks include: Increased heart rate, sudden changes in blood pressure, stomach pain, vomiting, headache, liver damage and reduced effectiveness
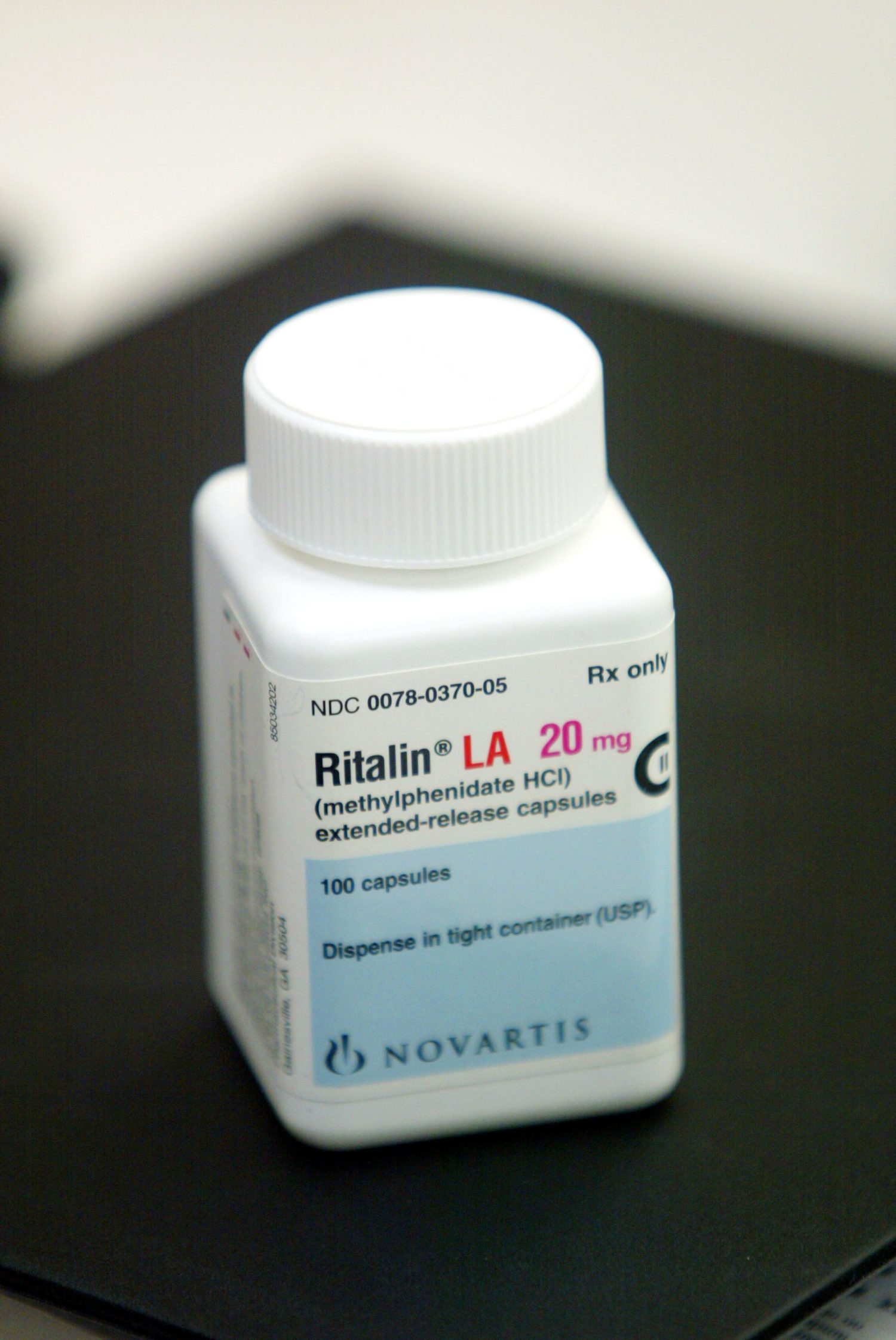
4. Attention-deficit medications (such as Adderall and Ritalin)
Risks include: Dizziness, drowsiness, impaired concentration and possible heart or liver damage
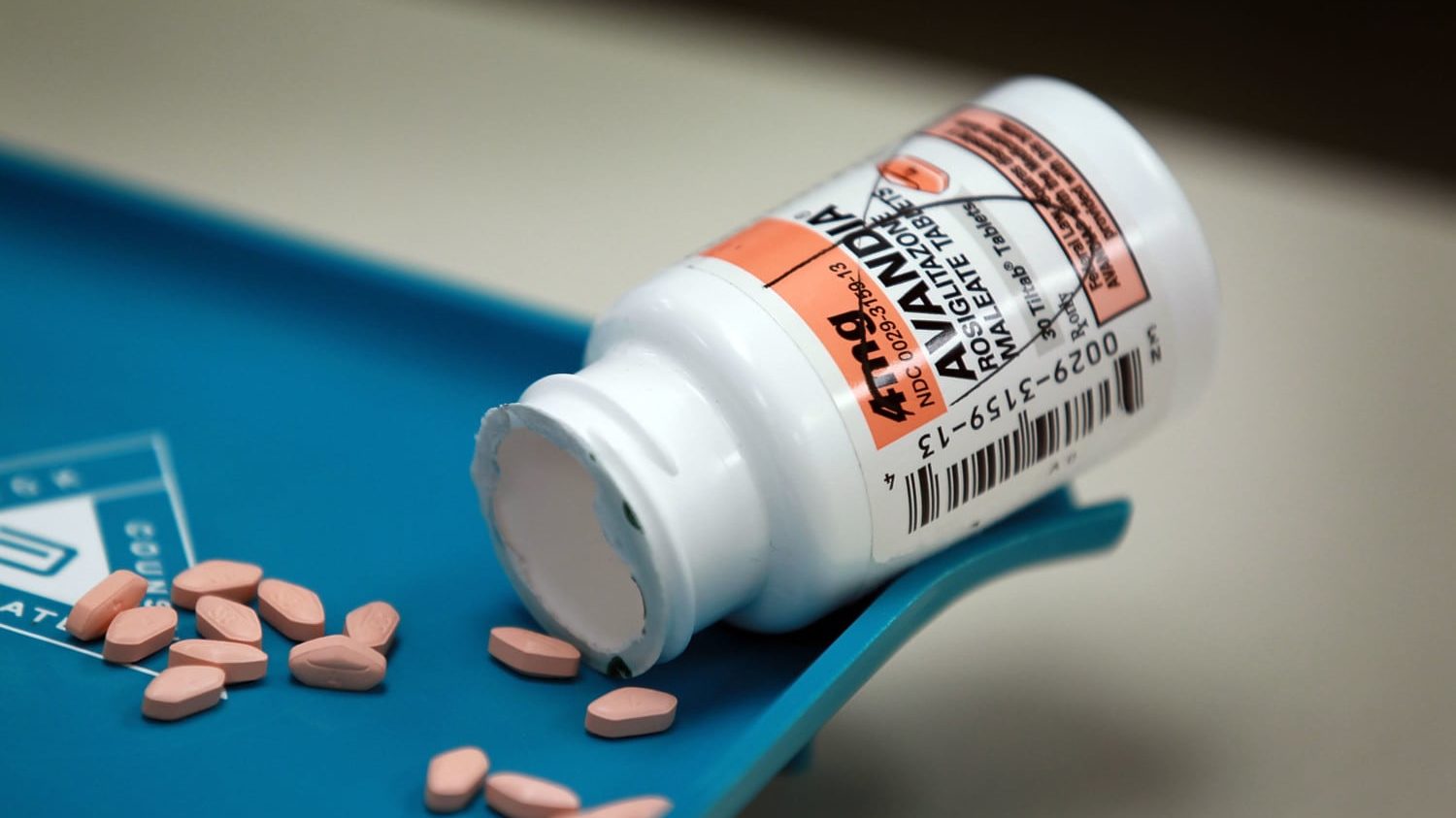
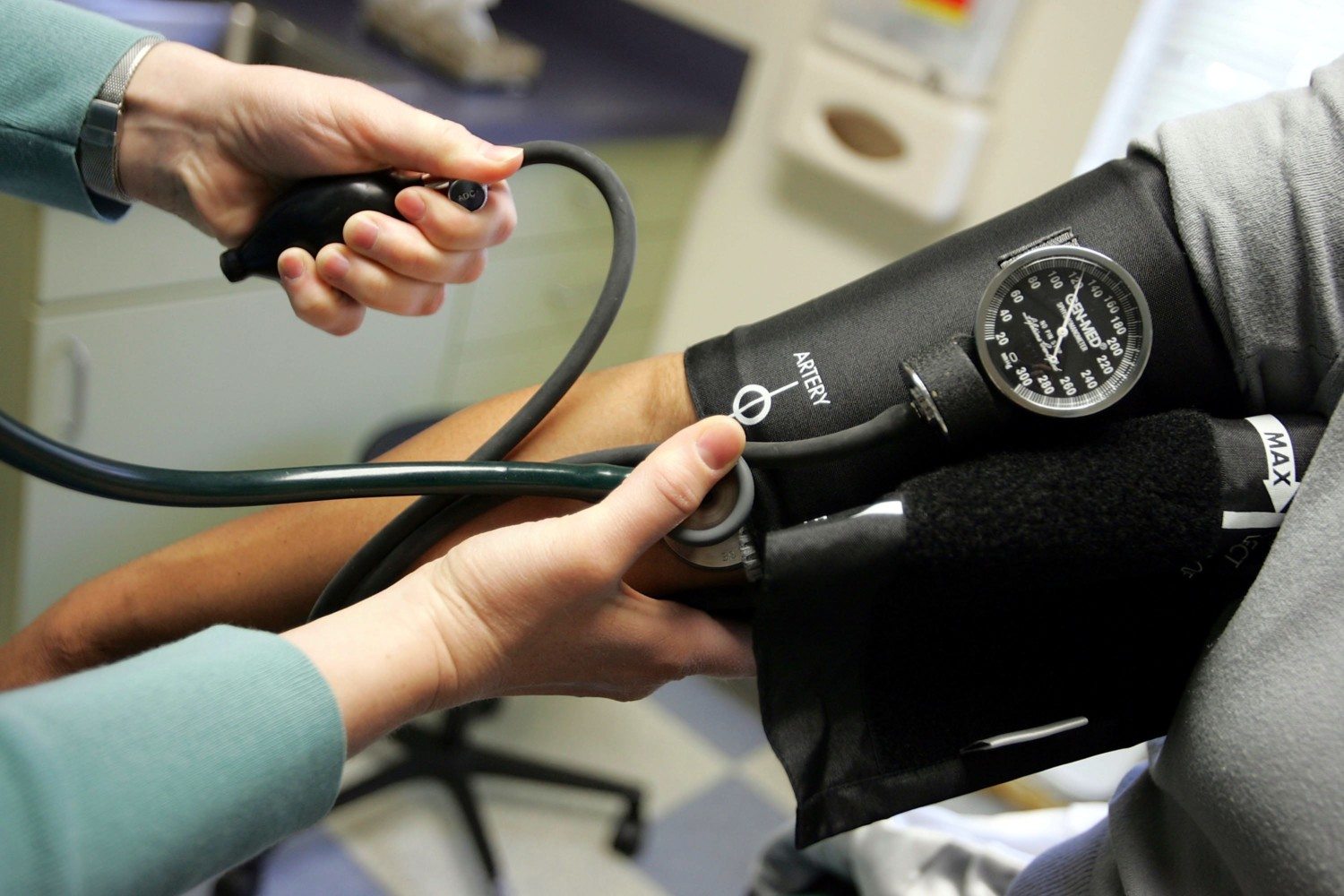
5. Blood pressure drugs
Risks include: Dizziness, fainting, drowsiness and heart problems, such as arrhythmia
6. Blood thinners
Risks include: Internal bleeding or an increased risk of blood clots, stroke or heart attack
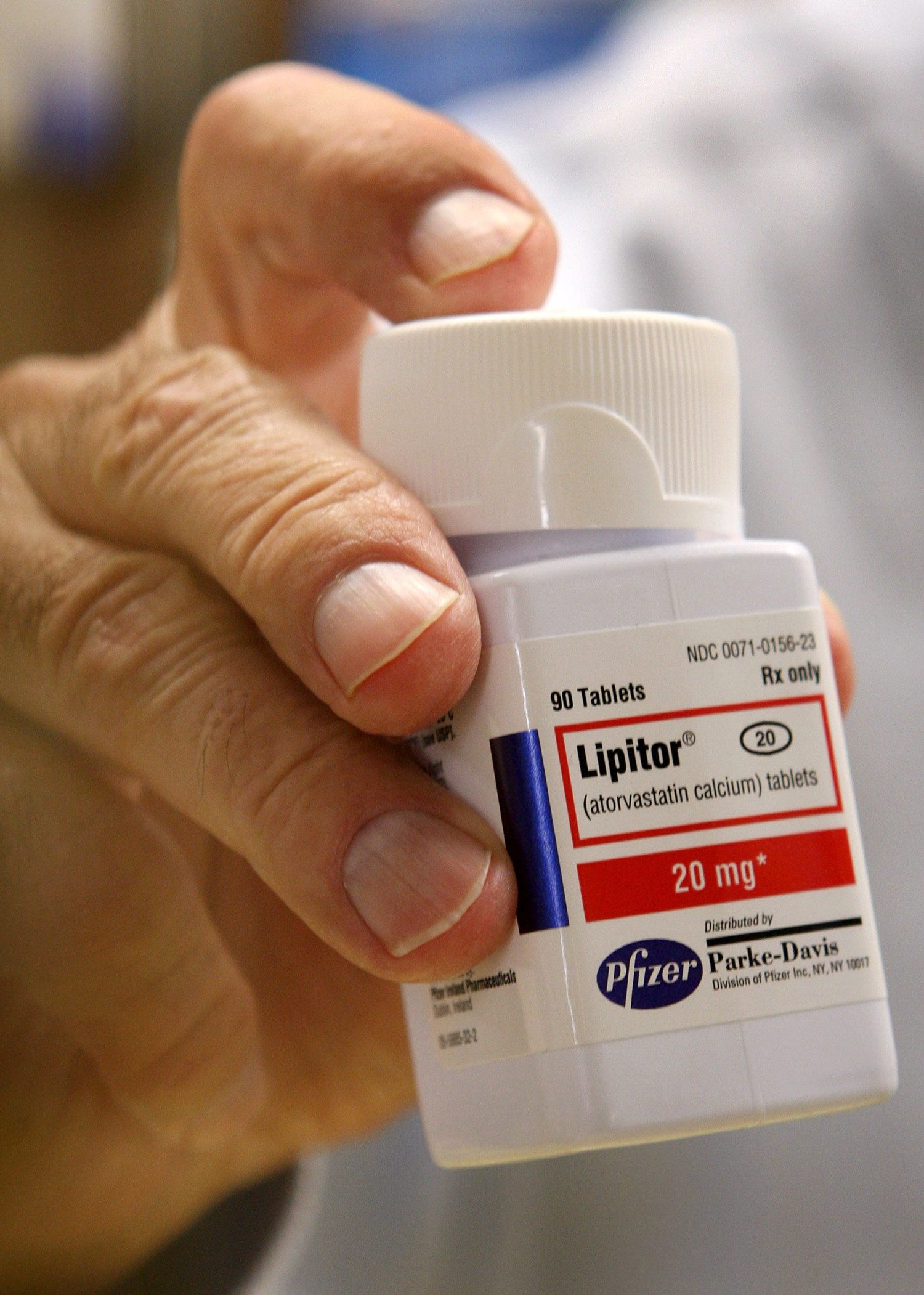
7. Cholesterol drugs (such as Lipitor)
Risks include: Liver damage, increased flushing and itching, increased stomach bleeding
RELATED: The Difference Between Advil, Tylenol, Aleve And Aspirin All Summed Up In One Chart
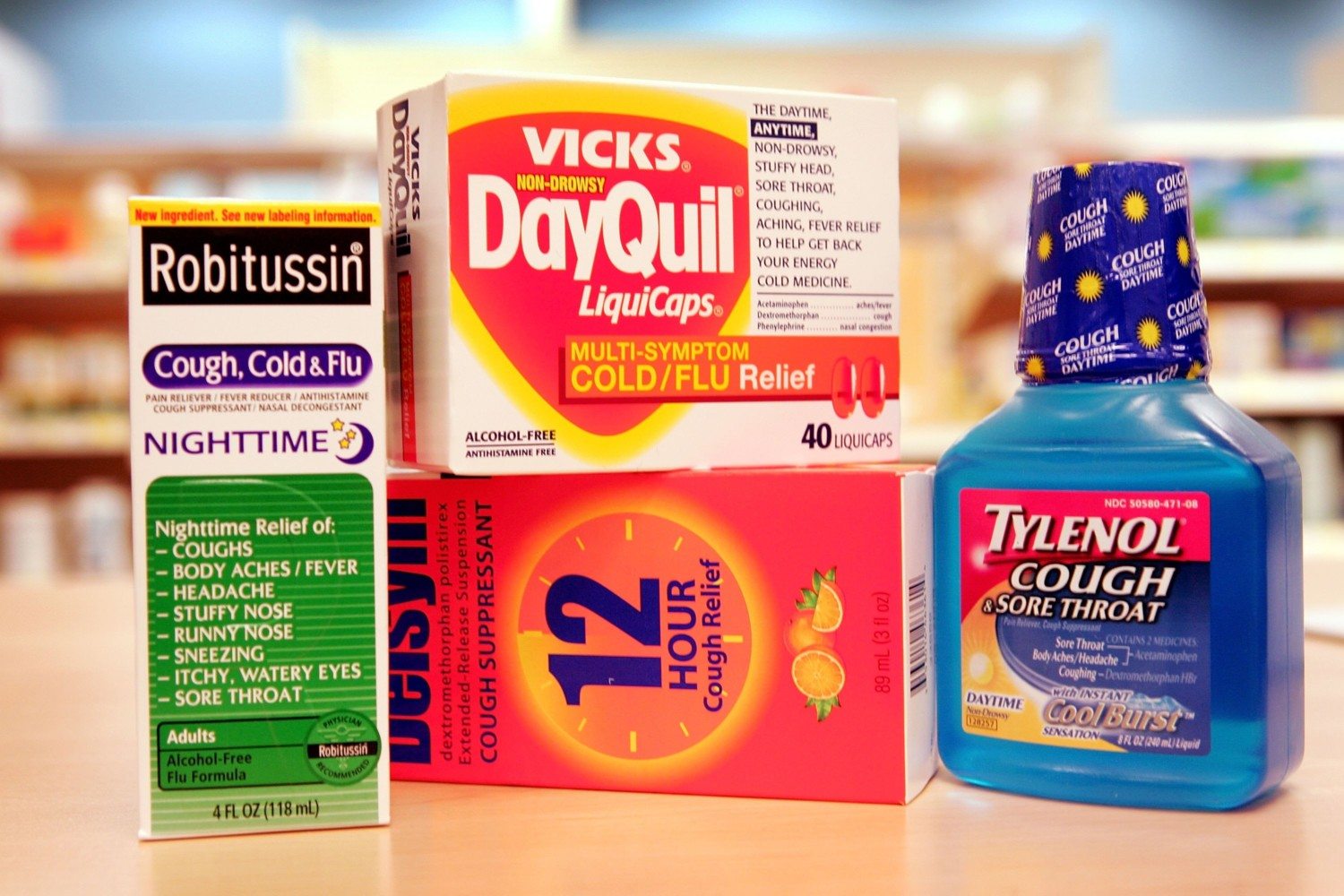
8. Cough medicine
Risks include: Drowsiness, dizziness and increased risk for overdose
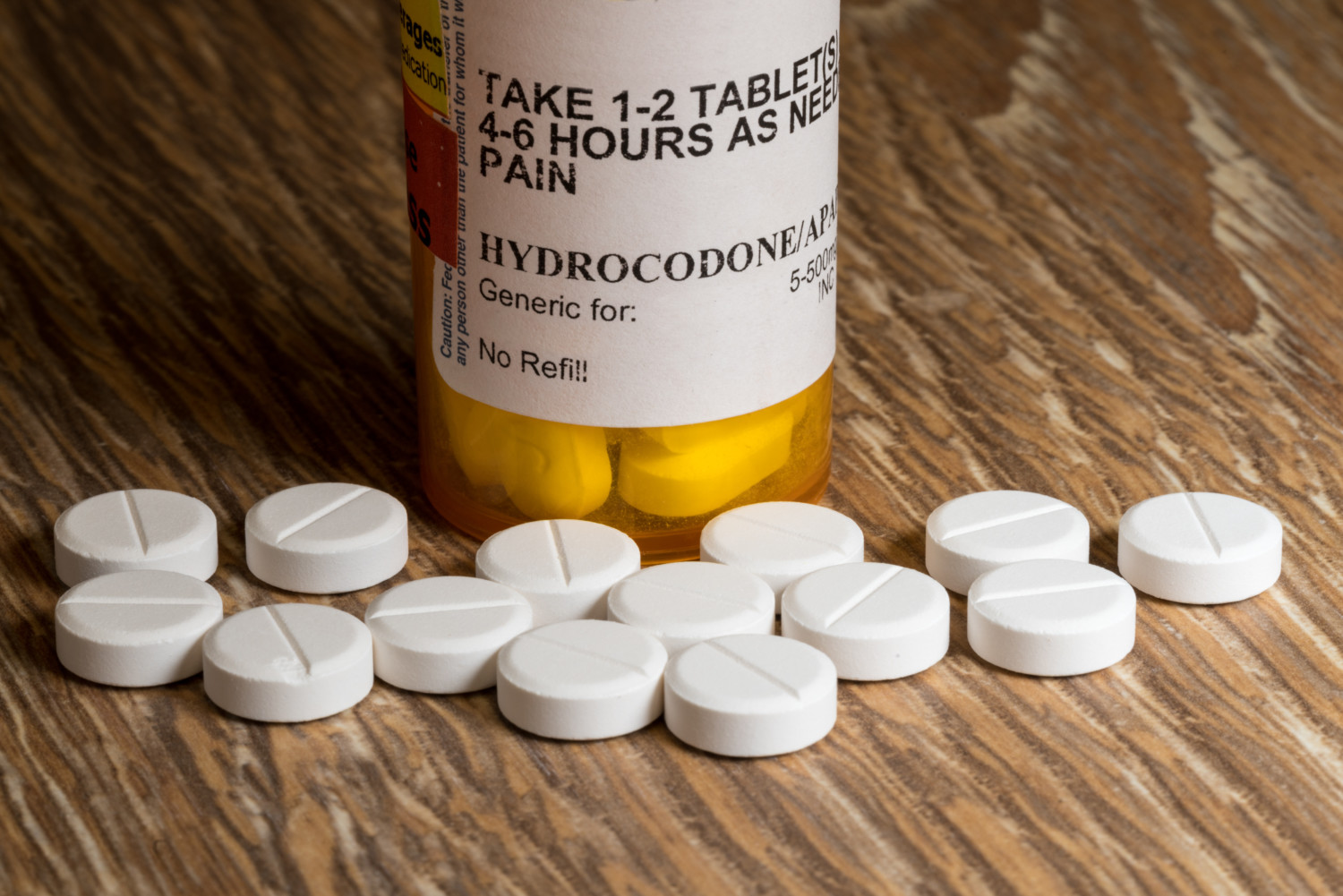
9. Prescription opioid pain relievers (such as Vicodin and Percocet)
Risks include: Drowsiness, dizziness, increased risk for overdose, slowed or difficulty breathing, impaired motor control, unusual behavior and memory problems
10. Over-the-counter pain relievers (such as Advil, Motrin, Aleve and Tylenol)
Risks include: Acetaminophen, the active ingredient in Tylenol, is a particularly bad medication to mix with alcohol, as it can lead to liver damage. Other risks include upset stomach, bleeding and ulcers and rapid heartbeat.
Women, Elderly At Greater Risk
As the NIH points out, while everyone should be following these guidelines, women and the elderly are at an even greater risk for some of the negative side effects of mixing alcohol with certain medications.
Women’s bodies have less water than men’s do, so the rate at which women process alcohol is slower. Likewise, our bodies are slower to process alcohol as we age. So the elderly are at greater risk because of this. Also, the elderly are more likely to take medications.
The bad news for women and alcohol doesn’t stop with mixing medications. Recent studies have found that a drink a day is tied to an increased breast cancer risk and that even moderate drinking may alter our brains.
RELATED: Here Are The Worrying Risks Of Over-The-Counter Sleep Aids
Alcohol’s Effects On The Brain And Body
While the research is mixed on the health benefits and harmful effects of drinking alcohol, one thing is decidedly clear: Long-term, excessive alcohol use is terribly damaging to your brain and your body, with complications including the liver condition cirrhosis and dementia.
In the video below from Business Insider, Dr. Samuel Ball of the National Center on Addiction and Substance Abuse at Columbia University talks about some of the effects alcohol has on your health.
When in doubt, always consult your doctor about what is safe for you. And if you’re not sure, it’s best to limit your alcohol intake — better safe than sorry!