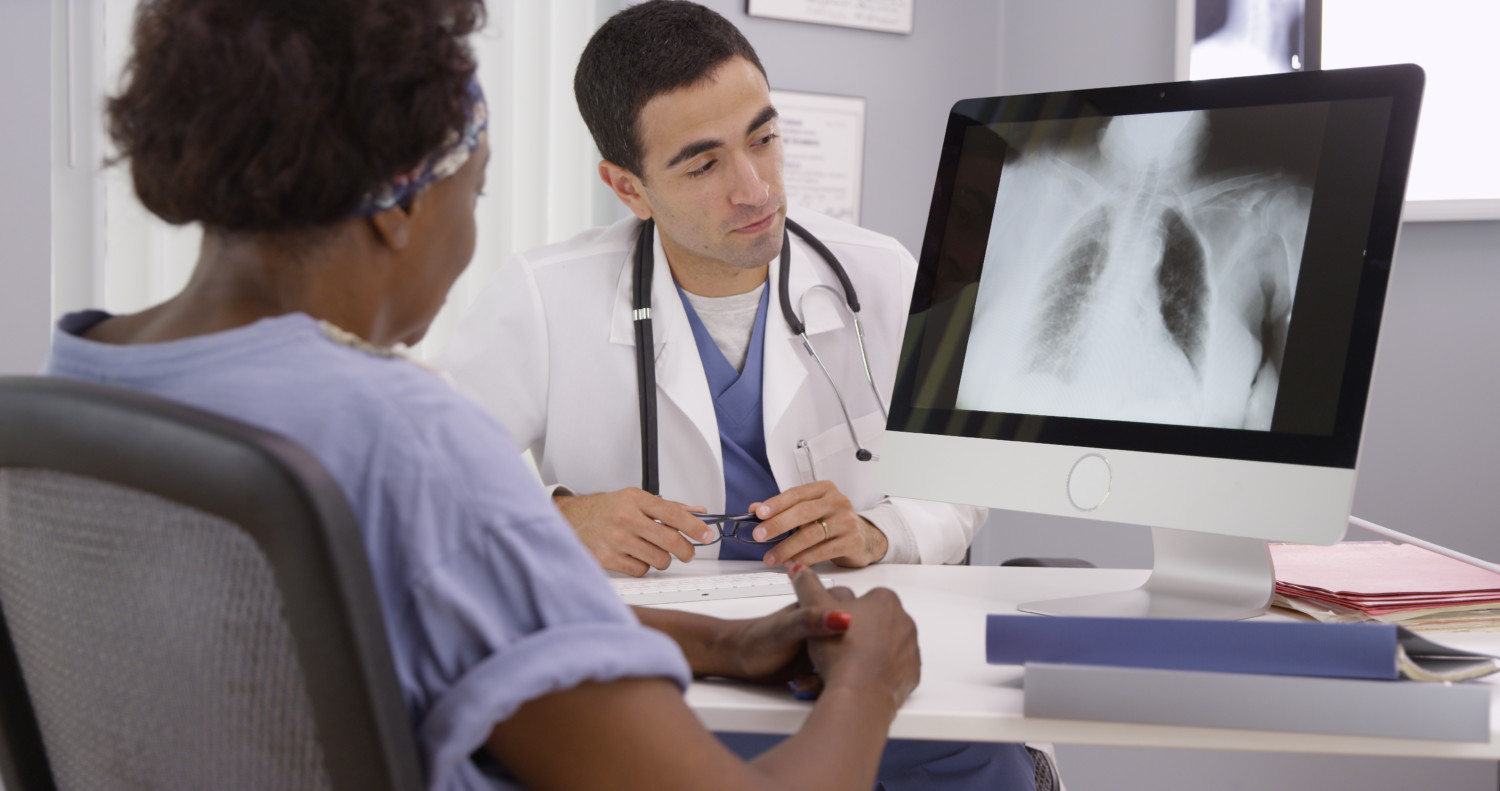
Lung cancer screening guidelines changed to include younger people who have smoked for fewer years
The guidelines for lung cancer screening have changed — and it means that the number of people in the United States who are advised to have annual CT scans for the illness will nearly double. The new recommendations from the U.S. Preventive Services Task Force, published recently in the medical journal JAMA, include people ages 50 to 80 who have smoked at least 20 “pack-years” (meaning that they have smoked a pack of cigarettes a day for 20 years, or an equivalent amount), and who still smoke or have quit within the past 15 years. So you could qualify if you’ve smoked a pack a day for 20 years or two packs a day for 10 years.
The recommended starting age for screening was lowered from 55 to 50, and the smoking history period of 20 years is 10 years shorter than in the previous guidelines, which were issued in 2013. The new criteria will qualify 14.5 million people in the United States for the screening, a huge increase of 6.4 million people.
Lung cancer is the leading cause of cancer deaths, killing 1.76 million people around the world in 2018, per the World Health Organization. That year, there were 2.09 million new cases of lung cancer. It’s also the leading cause of U.S. cancer deaths.
The new screening guidelines are designed to detect cancer early enough to cure it in more people who are at high risk because of smoking. According to the American Cancer Society, lung cancer is more likely to be successfully treated if it is found at an earlier stage, when it is small and before it has spread.
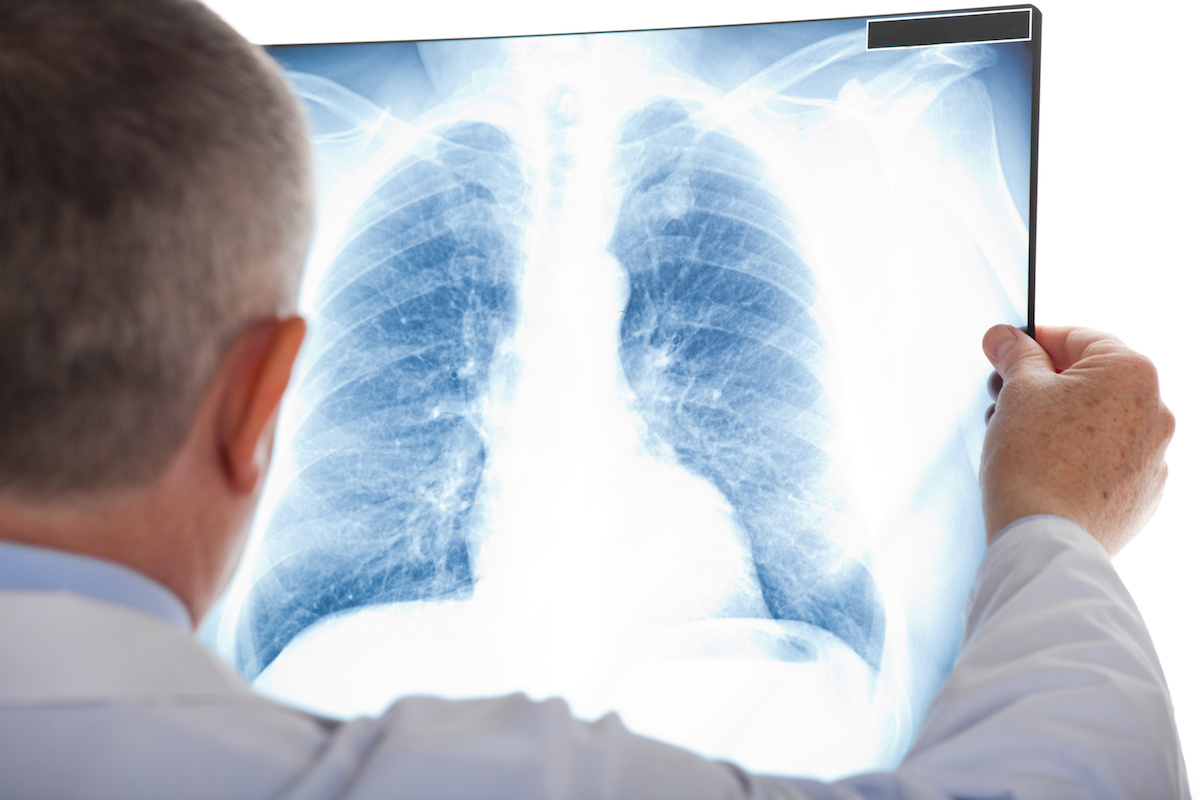
Lung cancer screening involves a type of chest computed tomography (CT) known as low radiation dose CT (LDCT). This uses reduced doses of radiation (compared to usual chest CT) to create extremely detailed 3D pictures of the lungs.
Studies have found that annual CT scans can reduce the risk of death from lung cancer by 20% to 25% in those individuals. The guidelines also mean many more women and Black Americans will be included than in the past. These groups may not have met the earlier screening threshold despite being at risk for lung cancer, because they tend to smoke less heavily than the white male study participants on whom earlier guidelines were based. Women and Black Americans also tend to develop lung cancer at an earlier age and from less tobacco exposure than white men.
“Some studies have alluded to some hormonal influences in women,” Dr. Mara Antonoff, a lung surgeon at the M.D. Anderson Cancer Center in Houston, told the New York Times. “In terms of racial differences, we don’t have an answer. We have population-based data to show they have a tendency to develop lung cancer younger and with less exposure to tobacco, but we don’t have a mechanism.”
Cancer specialists have welcomed the revised guidelines, but have also expressed some reservations over equality.
“Unfortunately, lowering the age and pack-year requirements alone does not guarantee increased equity in lung cancer screening,” wrote Dr. Yolonda Colson and colleagues at Massachusetts General Hospital in JAMA Surgery. Dr. Colson’s team pointed to “formidable” barriers, including poor access to healthcare and doctors who don’t know enough about the screening process to identify suitable candidates and aid their decision-making process.
A study published in 2019 analyzed trends in lung cancer screening in the United States from 2016 to 2017 and found that the overall rate of eligible patients who underwent screening was low. The authors concluded that the rate of lung cancer screening is slowly increasing with time, though most eligible patients are not screened.
Remember, quitting smoking is the best way to reduce the risk of dying from lung cancer — and screening isn’t a substitute for that.